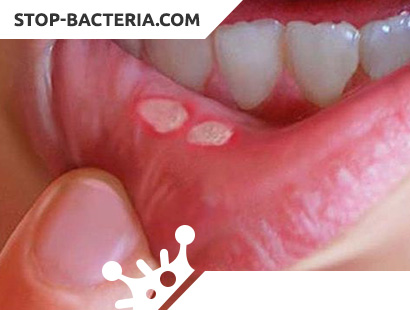
What is Acute Herpetic (Aphthous) Stomatitis?
Acute herpetic (aphthous) stomatitis is an acute contagious infectious disease that occurs with symptoms of general toxicosis of the body and local lesions of the oral mucosa. At the same time, there are violations on the part of the immunological system, the absence or inhibition of specific and nonspecific immunity factors. Herpes infection should be considered as a serious disease that occurs in violation of the immune, reticuloendothelial and nervous systems.
Causes of Acute Herpetic (Aphthous) Stomatitis
The causative agent of acute herpetic stomatitis is herpes simplex virus (HSV).
By antigenic properties of the virus is divided into 2 types. Type 1 – herpetic lesions on the oral mucosa, type 2 – lesion of the genital organs. The virus is DNA-containing. In the body, it multiplies in epithelial cells. Having entered the child’s body and causing manifestations of a primary herpetic infection, it remains in the latent state of a person’s life or causes a relapse of the disease (recurrent herpetic stomatitis). The virus is found in 75-90% of the adult population. Primary infection occurs more often at the age of 1-3 years, when the amount of antibodies received from the mother in the child’s blood disappears or decreases, and the body becomes susceptible to infection with the virus.
Pathogenesis during Acute Herpetic (Aphthous) Stomatitis
The source of infection is a sick person or a virus carrier (close relatives, attendants, children with acute herpetic stomatitis and recurrent herpetic stomatitis).
Cases of 6–10-month-old infants artificially fed from the first months of life have become more frequent. The disease is severe in newborns, especially contagious for people not previously infected with the virus.
Thus, studies indicate a relatively high incidence of acute herpetic stomatitis among children. The results confirm the data on the delay in recovery of the immunological reactivity of the organism in acute herpetic stomatitis from the time of clinical recovery.
The analysis showed that among patients there is a high percentage with moderate and severe forms of acute herpetic stomatitis, with long-term illness. Therefore, the treatment of acute herpetic stomatitis should be reduced not only to the treatment of stomatitis, but also the whole body with the participation of many specialists (pediatrician, dentist, immunologist, neuropathologist, etc.). Radical treatment should be directed not only at the epithelization of the elements of the lesion on the oral mucosa, but mainly at normalizing the indices of nonspecific immunity, restoring the body’s defenses.
Children suffering from acute herpetic stomatitis, especially moderate and severe form, are subject to constant monitoring by a pediatrician.
After the virus enters the body of the child, its reproduction occurs in the cells of local tissues and the nearest lymphatic formations; therefore, the appearance of lesion elements in the oral cavity is preceded by lymphadenitis of varying severity. The submandibular lymph nodes are usually involved in the process and accompany the course of the disease. In the incubation period, primary viraemia is observed, i.e. penetration of the virus into the bloodstream. Penetrating through the capillary barrier by diapedesis, the HSV is deposited in the liver, spleen and other organs and multiplies rapidly. There are lesions of tissues by type of foci of necrosis.
Secondary viremia corresponds to the prodromal period of the disease and the first days of its peak and is characterized by the appearance in the blood of a high level of the virus after its multiplication in the indicated organs. During secondary viremia, viruses infect the skin, mucous membrane, where their intracellular reproduction continues.
The catarrhal period is caused by generalized damage to epithelial tissues and the reproduction of HSV in them. The pathological process, depending on the degree of generalization, involves the mucous membrane of the oral cavity, pharynx, upper respiratory tract, eyes, genitals.
The more severe the disease, the more pronounced viremia and the intensity of intracellular reproduction of HSV, the longer and brighter the manifestation of catarrh of the mucous membranes. Under the influence of this process, a layer of secondary infection occurs, manifested by laryngitis, runny nose, cough, conjunctivitis, vulvitis.
The body’s immunological defense against HSV aggression is carried out through nonspecific and specific mechanisms:
- phagocytosis of infected viral cells;
- interferon production;
- the formation of antibodies;
- febrile reaction.
Children who have had acute herpetic stomatitis become asymptomatic carriers of the virus or suffer from recurrent herpetic stomatitis.
Virus interpolation of DNA from the DNA of neuronal nuclei protects the virus from the effects of antibodies, chemotherapy and cellular immune factors, ensuring the latency of infection.
Latency ensures the preservation of the virus in the host’s body until conditions are created that are favorable for the activation and transition of the virus to the infectious form, which leads to a relapse, i.e. under the influence of various factors, the balance of the organism / virus is disturbed in favor of the virus, which is reactivated and a relapse begins.
The factors leading to the recurrence of the disease include: violation of the humoral and cellular link of immunity, a decrease in the level of immunoglobulins, immunosuppressive and hematological disorders, the use of large doses of antibiotics, immunosuppressants and steroids. Exacerbation is also caused by factors such as local trauma, hypothermia, overheating, sun exposure, stress and fever, hormonal changes, as well as contact with a person who has manifestations of herpes infection.
The possibility of developing recurrent herpes is available if the score is equal to or greater than 6. The greater the amount, the greater the risk of the disease.
When the organism is infected with HSV, the protective role is played by specific and nonspecific humoral and cellular factors of immunity associated with the participation of antibodies, macrophages, lymphocytes, leukocytes, interferon. Recurrent herpetic stomatitis occurs against the background of suppression of the specific and nonspecific reactivity of the body.
The study of factors of humoral immunity in children with recurrent herpetic stomatitis reveals significant differences in comparison with adults. In case of recurrent herpes in children at the beginning of the chronicity of the disease, a specific immunobiological response in the form of the appearance of herpes antibodies in the serum is not always observed (only in 69.6% of cases). Subsequent relapses of the disease and repeated antigenic irritations lead to the fact that the overwhelming majority of sick children (84.7%) develop antiherpetic antibodies, i.e. relapses occur against the background of a high antibody titer.
Thus, the large role of immunological mechanisms in the pathogenesis of chronic recurrent herpes allows us to consider it not only a viral, but also to a large extent an immunological disease.
The process is difficult in the first months of life, when there is a generalization of damage to the mucous membrane, skin, eyes, etc. The generalized form is possible in a child born by a mother who does not have antibodies to the herpes simplex virus, they develop a septic state with damage to the serous membranes of the brain, internal organs. Extensive necrosis occurs in the oral cavity. Death is possible.
After recovering from primary herpes, the infection goes into a latent state and recurs under the influence of various factors. Infection occurs through direct contact with a patient with herpes or a virus carrier – contact or airborne infection. The incubation period lasts 2-17 days. In the development of the disease there are the following periods: prodromal, catarrhal, the period of rashes (the development of the disease), in which there are mild, moderate, severe forms of the disease, the period of extinction and clinical recovery (convalescence). Children aged 1-6 years get sick more often. The seasonality of acute herpetic stomatitis has been established in the spring and autumn months, it occurs more often than at other times of the year.
Symptoms of Acute Herpetic (Aphthous) Stomatitis
The incubation period lasts an average of 4 days. The disease begins acutely, as a rule, with an increase in temperature (37 – 41 ° C) and general malaise. After 1 – 2 days, there is pain in the oral cavity, aggravated by eating and talking.
The mucous membrane turns red and swells, then small vesicles, single or in groups, are poured on it, their number varies from 2 – 3 to several dozen. The stage of the vesicle is usually not fixed by the patient and the doctor, as it quickly turns into erosion. Surface erosion has a round, oval or slit-like shape, smooth edges, a smooth bottom, covered with a grayish-white fibrinous bloom. Erosions can turn into superficial ulcers, and with the addition of a secondary infection, into deeper necrotic ulcers. Erosion is localized mainly on the palate, tongue, lips.
Regional lymphadenitis precede the appearance of aft-erosions, accompany the disease and persist for another 5-10 days after the epithelialization of erosions. Often, the red border of the lips and surrounding areas of the skin, and sometimes the skin of the hands, are affected. The process may involve other mucous membranes, primarily the gastrointestinal tract.
The disease has a favorable prognosis, clinical recovery occurs after 1 – 3 weeks, aphthae heal without scarring, the edges of the gums retain their shape. By the severity of the course, there are mild, moderate and severe forms. The severity of the disease is assessed mainly by the severity of toxicosis and the area of damage to the oral mucosa.
Diagnostics of the Acute Herpetic (Aphthous) Stomatitis
Diagnosis of herpetic stomatitis is a difficult task and is based on the use of special molecular biological, virological, serological, cytological and immunological studies.
In the blood, nonspecific changes characteristic of an acute inflammatory process are found. The saliva pH value shifts first to the acidic, then to the alkaline side. In saliva, the content of lysozyme is reduced, interferon is absent.
Histological examination is characterized by intraepithelial arrangement of vesicles (in the lower layers of the styloid layer), acantholysis of epithelial cells, ballooning and lenticular degeneration, an acute inflammatory process is expressed in the underlying mucous membrane itself.
In cytological examination, the predominance of histiocytes, neutrophils, layers of epithelial cells, often with the phenomena of polymorphism and in the form of syncytia, is noticeable. The appearance of giant multinucleated cells (30 – 120 µm in diameter), characterized by sharp polymorphism in size, shape and color, is characteristic. The nuclei – from 2 – 3 to several hundred – are located in the center in the form of a dense conglomerate or (less often) separately. Nucleoles are usually not visible. In acute herpetic gingivostomatitis, there are few such cells and they are not always found.
For the diagnosis of acute herpetic stomatitis, the method of immunofluorescence, electron microscopy is used.
With acute herpetic stomatitis in the first days of the disease, as well as during relapses, the herpes virus is easily excreted from the contents of the vesicles. However, during the period of remission, it is not possible to detect the virus in the skin and mucous membranes. At the onset of the disease, antibodies to the virus are not detected. Then their titer gradually increases. After clinical recovery, the herpes virus remains in the body, as a rule, for life. Unstable non-sterile immunity arises.
Differential diagnosis is carried out with other viral diseases: vesicular stomatitis, herpangina, foot and mouth disease, as well as with allergic lesions and exudative erythema multiforme. Differentiation with vesicular stomatitis is possible only with the use of virological research methods.
Herpangina differs in the localization of the lesion – rashes in the oropharynx. Dysphagia, myalgia are possible. The results of virological studies for these two diseases are different.
In differential diagnosis with foot and mouth disease, attention should be paid to the epidemiological situation, to the possibility of typical skin lesions. Objectively, the diagnosis of foot and mouth disease is confirmed by the setting of biological samples in an infectious diseases hospital, as well as by the results of serological studies, the isolation of the virus. Hypersalivation is an important clinical sign of foot and mouth disease.
Allergic bullous erosive lesions and exudative erythema multiforme differ in history, morphological elements of the lesion (subepithelial blisters, then large erosions), as well as the results of allergic tests and virological studies.
Treatment of Acute Herpetic (Aphthous) Stomatitis
Acute herpetic stomatitis can be cured spontaneously, but treatment promotes an easier course, accelerates recovery, eases the suffering of the patient, and prevents complications. The volume and nature of therapeutic measures depend on the stage of the disease, the severity of the course, and secondary infection.
General therapy. The antiviral drug Bonafton is prescribed 0.1 g 3 – 5 times a day in cycles of 5 days with intervals of 1 – 2 days. In order to detoxify, hyposensitize and increase the body’s defenses, sodium salicylate is used (for adults, 0.5 g 4 times a day), antihistamines (diphenhydramine, suprastin, diazolin, etc.) in medium therapeutic doses, calcium gluconate 0.5 – 1.0 g 3 times a day, vitamins, especially C and P. In a hospital setting, 25-50 μg of prodigiosan is successfully used 2-3 times with an interval of 3-4 days, intramuscular lysozyme. In a severe form of the disease, especially if it is complicated by fusospirochetosis, metronidazole or broad-spectrum antibiotics are prescribed orally (children, during the formation of teeth, should not be given tetracycline antibiotics), if indicated, cardiovascular agents. A diet is mandatory – crushed high-calorie fortified food, drinking plenty of fluids.
Antiviral and immunocorrective drugs are effective. Leukinferon is prescribed by inhalation and daily intramuscular injections. The course of treatment is 7-10 days. Acyclovir (Zovirax) is used 1 tablet (0.2 g) 4 times a day, the course is 5 days. Imudon – 6 – 8 sublingual tablets per day – for 14 – 21 days; interferon – intranasally – 5-6 drops 3 times a day for a week.
Local therapy. In the first days of rashes, antiviral drugs are prescribed – interferon in the form of a solution or ointment (interferon – 1 ampoule, anhydrous lanolin – 5 g, peach oil – 1 g, anesthesin – 0.5 g), 0.5% bonafton, 1 – 2% Florenal or 2% tebrofen ointment, 3% liniment of gossypol, etc. These drugs are applied to the entire mucous membrane after preliminary treatment with proteolytic enzymes, antiseptics or herbal decoctions (chamomile, sage, tea). The oral cavity is also treated with proteolytic enzymes once a day. Of the enzymes, it is advisable to use a 0.2% solution of deoxyribonuclease, which is characterized by antiviral and lysing action.
Throughout the course of the disease, antiseptic agents are used locally: in adults – in the form of rinsing and baths of the oral cavity, in young children – in the form of rinsing the oral cavity with a rubber pear or aerosols in the prone position. Use warm solutions of potassium permanganate (1: 5000), 0.25 – 0.5% hydrogen peroxide, 0.25% chloramine, furacilin (1: 5000), 0.1% chlorhexidine, etc. Pain relievers are required. Especially widely used 5 – 10% solution of anesthesin in peach or other oil, 1% solution of trimecaine, 1 – 2% solution of pyromecaine, 10% aerosol of lidocaine.
In order to enhance the regeneration and epithelization of the mucous membrane, an oil solution of vitamin A, carotolin, aloe liniment, rosehip oil, Shostakovsky’s balsam, dental adhesive paste with solcoseryl are recommended. Aerosols are especially convenient. From the first day of the patient’s treatment and until complete epithelialization, physiotherapy is used: UF-irradiation, laser therapy. Erosion on the skin is treated for the first 2 – 3 days with antiviral drugs, then with zinc ointment or Lassar paste, with impetiginization – with antibiotic ointments.
Prevention of Acute Herpetic (Aphthous) Stomatitis
Isolation of the patient (sick children are not allowed to visit children’s institutions until the erosion is completely epithelized). In children’s institutions, persons with clinical manifestations of herpes infection of any form and localization should not be allowed to work with children.
In the treatment of acute herpetic stomatitis, along with dentists, pediatricians, immunologists, neuropathologists and other specialists should take an active part.