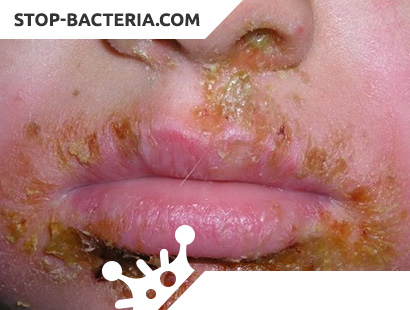
What is Impetigo in Children?
Impetigo is an abscess disease that causes staphylococci or streptococci.
Impetigo strikes children’s groups – for example, kindergartens, nurseries (often), orphanages. Both home and school outbreaks can occur. Impetigo is a dangerous disease because it causes complications that affect the internal organs. Therefore, any outbreak of impetigo in children should be investigated – look for the causes and sources of infection, and children are treated.
Causes of impetigo in children
Infetigo leads to infection by two types of bacteria – Staphylococcus aureus or acute streptococcus. These two types of bacteria grow and multiply where large groups of people come in contact. This is especially true for schools and kindergartens. Staphylococcal and streptococcal bacteria are not dangerous until they penetrate the body through a wound, leading to infection of the body.
Risk factors for impetigo:
- Summer and the rainy season
- Countries with subtropical and tropical climates
- Poor sanitation, war, epidemics
- Minor skin damage, microtrauma, insect bites
- Weak immunity due to anemia, hypovitaminosis, malnutrition
- The presence of sick impetigo family members
- Contact dermatitis
- Impetigo can be a complication of scabies, pediculosis, chickenpox, eczema
- Metabolic disorders, for example, diabetes
Symptoms of Impetigo in Children
With staphylococcal dermatitis in children, pustules the size of millet grain appear on the skin. The base of the abscess is red, and a hair grows in its center. The skin between the pustules is not red, without changes, there is no soreness, no itching. After a week (maximum – 9 days), the pustules disappear without leaving scars.
Streptococcal impetigo is more characteristic of childhood. On the skin of the eyelid, superficial vesicles not associated with the hair sac are found, the size of which can be both with a pin head and lentils. The vesicle contains transparent (sometimes turbid or hemorrhagic) contents. The bubbles open and crusts form in their place. After 8-14 days, the crusts disappear, in their places the skin takes the form of bluish-red spots. The process may affect the conjunctiva.
The third type of impetigo in children is mixed – streptococcal + staphylococcal infection. This species is also known as vulgar impetigo. Purulent contents are observed in the vesicles, massive crusts are formed. Vulgar impetigo most often occurs on the skin of the face, less often on the body, arms and legs. Multiple rashes are observed. If adequate timely treatment is not carried out, new rashes form near the past rashes or in other areas, the process is often widespread. After peeling, the surface of the skin is moist and eroded. The infection is transmitted to new areas of the skin through the hands and underwear. Regional lymph nodes become painful on palpation and somewhat swollen.
Complications
Impetigo often ends without complications, with a successful outcome. But complications are also likely. Impetigo can cause complications in the kidneys – nephritis occurs, as well as in the heart – it causes myocarditis. Staphylococcal impetigo can have complications such as abscesses and phlegmon – common purulent processes.
Diagnosis of Impetigo in Children
It is easy to diagnose impetigo in children – a typical clinical picture and a corresponding anamnesis. In the most difficult cases, a microbiological examination of the discharge is necessary.
Differential diagnosis of bullous impetigo with diseases characterized by vesicular and bullous rash:
Nosological form – Main clinical signs – Methods of confirmation
Bullous impetigo – Acute onset, flabby blisters with transparent contents appear in the skin folds. It provokes the disease Staphylococcus aureus – Clinical picture. In difficult cases, inoculation of the contents of the bladder or material from the crust is used.
Bullous pemphigoid – The appearance of tense blisters, the size of which is 1-2, the background skin is normal or erythematous, urticular plaques – Histology of the bladder in order to confirm its formation at the level of the subepidermal plane and to identify the accumulation of eosinophils in the dermis. Immunopathological research.
Herpes zoster – Acute onset with maculopapular eruptions arranged in clusters that quickly become vesicles, then darken and dry out, leaving crusts behind.
Insect bites (bullous) – A group of tense blisters in the area of the bite. Blisters larger than 1 cm and surrounded by skin without changes – Clinical picture.
Stevens-Johnson Syndrome – Loose blisters and vesicles that form in the center of the target elements. Bubbles open quickly, weeping erosion remain in their place – Histological examination.
Congenital syphilis – Bubbles are located only on the palms and feet. They are small in size, the skin is crimson-red against the background. There are spots and papules – A clinical picture. It is accompanied by rhinitis, cracks in the corner of the mouth and eyes, diffuse infiltrates, bright red-pink spots.
Treatment of Impetigo in Children
While the treatment is underway, the affected skin should not be moisturized with water. A sick child is recommended a hypoallergenic diet and general vitamin therapy. The skin on which the rash is visible is lubricated with 0.1% camphor alcohol or 2% salicylic alcohol two or three times a day. Then they resort to using antibacterial ointments, and then apply a sterile bandage using:
- tetracycline 1% ointment
- erythromycin 1% ointment
- Colbiocin ointment
- Oriprim-P ointment and Ophthalmite.
When the bubbles have opened, and erosion has formed in their place, the surface of the skin must be treated with dyes and antiseptics:
- methylene blue 1% alcohol solution;
- brilliant green 1% alcohol solution;
- iodine 2% alcohol solution;
- potassium permanganate 1% solution;
- furacilin 1: 5000 solution.
Antimicrobial solutions are instilled into the conjunctival sac for 1-2 weeks three times a day, for example, picloxidine solution, miramistin solution, chloramphenicol solution, sodium sulfacyl solution.
For 7-10 days, antibacterial ointments are placed in the conjunctival sac before going to bed:
- erythromycin 1% ointment;
- tetracycline 1% ointment;
- Fucitalmic;
- Colbiocin ointment;
- Oriprim-P ointment and Ophthalim.
With widespread impetigo or its transition to the tissue of the conjunctiva, doctors prescribe systemic antibacterial drugs inside:
- cephalexin
- oxacillin
- erythromycin
- cefadroxil.
Autohemotherapy is also used to treat impetigo in children.
Evaluation of the effectiveness of treatment
If the diagnosis and treatment is carried out on time, the child will fully recover. If therapy is carried out untimely or there is a relapse, there may be cicatricial changes in the eyelids and impaired growth of eyelashes (if the edge of the eyelid is affected).
Prevention of Impetigo in Children
Preventive measures – treatment of diseases that can lead to impetigo, adherence to the rules of personal hygiene, treatment of small and microtraumas with antiseptics. Children with impetigo are treated at home, isolated from other children. In children’s institutions, systematic sanitary and epidemic supervision is necessary.