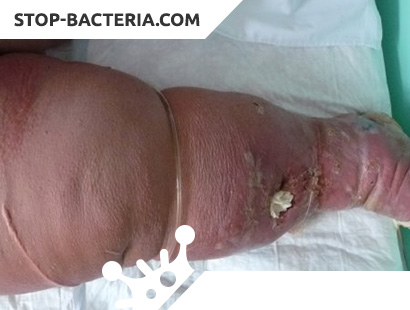
What is Erysipelas?
Erysipelas is an infectious disease characterized by the appearance on the skin or mucous membranes of foci of clearly demarcated acute serous or serous-hemorrhagic inflammation, fever and symptoms of general intoxication. The disease is prone to recurrent course.
Brief historical information
Erysipelas has been known since ancient times. In the writings of ancient authors, it is described under the name erysipelas (Greek: erythros – red + lat. Pellis – leather). The work of Hippocrates, Celsius, Galen, Abu Ali Ibn Sina is devoted to the issues of the clinic, differential diagnosis and treatment of erysipelas. In the second half of the XIX century N.I. Pirogov and I. Zemmelweis described the outbreaks of erysipelas in surgical hospitals and maternity hospitals, considering the disease highly contagious. In 1882, I. Feleizen received for the first time a pure streptococcus culture from a patient with erysipelas. As a result of the subsequent study of the epidemiological features and pathogenetic mechanisms, the success of chemotherapy, erysipelas with sulfonamides and antibiotics, the concept of the disease has changed, it has been attributed to the category of sporadic low contagious infections. A great contribution to the study of the problems of erysipelas in the Soviet era was made by E.A. Halperin and V.L. Cherkasov.
Causes of Erysipelas
The causative agent is group A streptococcus (S. pyogenes), which has a complex set of antigens, toxins and enzymes.
Epidemiology
The reservoir and source of infection is a person with various forms of streptococcal infection (caused by Streptococcus group A) and a “healthy” carrier of Streptococcus group A.
The mechanism of transmission is aerosol, the main route of infection is airborne, but contact infection is also possible. Entrance gates are various injuries (injuries, diaper rash, cracks) of the skin or mucous membranes of the nose, genitals, etc. Streptococcus group A often colonizes the surface of the mucous membranes and skin of healthy individuals, so the risk of infection with erysipelas is great, especially with elementary untidiness.
Natural susceptibility of people. The occurrence of the disease is probably determined by a genetically determined individual predisposition. Among the diseased women prevail. In individuals with chronic tonsillitis and other streptococcal infections, erysipelas occurs 5-6 times more often. Local factors predisposing to the development of facial erysipelas are chronic diseases of the oral cavity, caries, and diseases of the upper respiratory tract. The erysipelas of the chest and limbs most often occurs in lymphedema, lymphovenous insufficiency, edema of various origins, mycosis of the feet, and trophic disorders. Post-traumatic and postoperative scars predispose to localization of the lesion in the place of its location. Increased susceptibility to the face can be caused by prolonged use of steroid hormones.
Major epidemiological signs. I give birth to the most common infections of a bacterial nature. Officially, the disease is not registered, therefore, information on the incidence is based on selective data.
Infection can develop both exogenously and endogenously. Face mucus can be the result of lymphogenous drift of the pathogen from the primary lesion in the tonsils or the introduction of streptococcus into the skin Despite the rather wide spread of the pathogen, the disease is observed only in the form of sporadic cases. Unlike other streptococcal infections, the erysipelas does not have pronounced autumn-winter seasonality. The greatest incidence observed in the second half of summer and early autumn. People of different professions suffer from erysipelas: builders, employees of “hot” workshops and people working in cold rooms often suffer; for workers of metallurgical and coke-chemical enterprises, streptococcal infection becomes an occupational disease.
It should be noted that if in 1972-1982. the clinical picture of erysipelas was distinguished by the prevalence of moderate and light forms, then in the next decade there was a significant increase in the proportion of severe forms of the disease with the development of infectious-toxic and hemorrhagic syndromes. Recently (1995-1999), light forms make up 1%, medium-heavy ones – 81.5%, severe ones – 17.5% of all cases. The proportion of patients with erysipelas with hemorrhagic syndrome reached 90.8%.
Pathogenesis during Erysipelas
When exogenous infection, the pathogen is introduced through damaged skin (abrasions, scratches, wounds, diaper rash, cracks), as well as mucous membranes. In the presence of foci of chronic streptococcal infection in the body with periodic reversal of L-forms of streptococcus into bacterial, endogenous introduction of the pathogen into the skin with blood flow is possible. Propagating in cutaneous lymphatic capillaries, streptococcus causes the formation of an active inflammatory or latent focus of infection in the dermis. In the latter case, the pathogen persists for a long time in the skin, transforming into intracellular parasitic L-forms, or spreads through the hematogenous organs of the mononuclear-phagocytic system, where its L-transformation also occurs. This process underlies the formation of persistent foci of chronic streptococcal infection. Subsequent reversal of the pathogen into bacterial forms determines the possibility of developing relapse of the disease.
With the active propagation of streptococci in the dermis, their toxic products (exotoxins, enzymes, components of the cell wall) penetrate the bloodstream. Toxinemia causes the development of an infectious-toxic syndrome with high fever, chills and other manifestations of intoxication. At the same time, short-term bacteremia develops, but its role in the pathogenesis of the disease has not been conclusively clarified.
In the skin or on the mucous membranes (much less often), a focus of infectious-allergic serous or serous-hemorrhagic inflammation is formed. A significant role in its development is played by the pathogenicity factors of streptococci that have a cytopathic effect: antigens of the cell wall, toxins and enzymes. Moreover, the structure of some human skin antigens is similar to the streptococcus A polysaccharide, which leads to the appearance of autoantibodies in patients with erysipelas that enter into autoimmune reactions with skin antigens.
Autoimmunopathology increases the level of an individual predisposition of the body to the effects of streptococcal antigens. In addition, immune complexes with pathogen antigens are formed in the dermis and papillary layer. Autoimmune and immune complexes can cause damage to the skin, blood and lymphatic capillaries, contribute to the development of intravascular coagulation with a violation of the integrity of the vascular wall, the formation of microthrombi, the formation of local hemorrhagic syndrome. As a result, hemorrhages or blisters with serous or hemorrhagic contents are formed in the focus of infectious-allergic inflammation with erythema and edema.
The pathogenesis of erysipelas is based on an individual predisposition to the disease. It can be congenital, genetically determined or acquired as a result of various infections and other diseases, accompanied by an increase in the body’s sensitization to streptococcal allergens, endoallergens, allergens of other microorganisms (staphylococci, Escherichia coli, etc.). In the presence of an individual predisposition, the body responds to the introduction of streptococcus into the skin by the formation of a delayed-type hypersensitivity with the development of serous or serous-hemorrhagic inflammation.
An important component of pathogenesis is a decrease in the activity of factors that determine the patient’s protective reactions: nonspecific protection factors, type-specific humoral and cellular immunity, local immunity of the skin and mucous membranes.
In addition, neuroendocrine disorders and an imbalance of biologically active substances (the ratio of histamine and serotonin content) play a role in the development of the disease. Due to the relative insufficiency of glucocorticoids and an increase in the level of mineralocorticoids in patients with erysipelas, a local inflammatory process with edema syndrome is supported. Hyperhistaminemia helps to reduce the tone of the lymphatic vessels, increase lymph formation, increase the permeability of the blood-brain barrier for microbial toxins. With a decrease in serotonin content, vascular tone decreases, microcirculatory disturbances in tissues increase.
Tropism of streptococci to the lymphatic vessels provides a lymphogenous pathway of dissemination with the development of lymphangitis, sclerosis of the lymphatic vessels with frequent repeated episodes of erysipelas. As a result, lymph resorption is disturbed, persistent lymphostasis (lymphedema) is formed. Due to the breakdown of the protein, fibroblasts are stimulated with the growth of connective tissue. Secondary elephantiasis (fibredema) is formed.
Morphological changes in erysipelas are represented by serous or serous-hemorrhagic inflammation of the skin with edema of the dermis, hyperemia of the vessels, perivascular infiltration of lymphoid, leukocyte and histiocytic elements. Atrophy of the epidermis, disorganization and fragmentation of collagen fibers, swelling and homogenization of the endothelium in the lymphatic and blood vessels are observed.
Symptoms of Erysipelas
The modern clinical classification of erysipelas provides for the allocation of the following forms of the disease.
- By the nature of local lesions:
– erythematous;
– erythematous-bullous;
– erythematous hemorrhagic;
– bullous hemorrhagic. - According to the degree of intoxication (severity):
– easy;
– moderate;
– heavy. - By the multiplicity of the current:
– primary;
– repeated;
– recurrent (often and rarely, sooner or later). - The prevalence of local manifestations:
– localized;
– common;
– wandering (creeping, migrating);
– metastatic.
Explanations for classification.
- Relapsing erysipelas includes cases that occur in the period from several days to 2 years after the previous disease, usually with the same localization of the local process, as well as later, but with the same localization with frequent relapses.
- Re-erysipelas include cases that occur no earlier than 2 years after the previous illness in persons who have not previously experienced recurring erysipelas, as well as cases that developed earlier, but with a different localization.
- Localized are the forms of the disease with a local focus of inflammation, localized within the same anatomical region, common – when the focus is captured by more than one anatomical region.
- Cases of the disease with the addition of phlegmon or necrosis (phlegmonous and necrotic forms of erysipelas) are considered as complications of the disease.
The incubation period can be established only with post-traumatic erysipelas, in these cases it lasts from several hours to 3-5 days. In more than 90% of cases, erysipelas begins acutely, patients indicate not only the day, but also the hour of its occurrence.
The initial period is characterized by a rapid rise in body temperature to high numbers, chills, headache, aching muscles and joints, weakness. In severe cases of the disease, vomiting, convulsions and delirium are possible. After a few hours, and sometimes on the 2nd day of illness, in a limited area of the skin, there is a feeling of bursting, burning, itching, moderate soreness, weakening or disappearing at rest. Pain is most pronounced with erysipelas of the scalp. Quite often, pain occurs in the region of regional lymph nodes, aggravated by movement. Then there is redness of the skin (erythema) with edema.
At the height of the disease, subjective sensations, high fever and other general toxic manifestations persist. Due to toxic damage to the nervous system against the background of high body temperature, apathy, insomnia, and vomiting may develop, with hyperpyrexia – loss of consciousness, delirium. A spot of bright hyperemia with clear uneven borders in the form of “tongues of flame” or “geographical map”, edema, and skin tightening forms on the affected area. The focus is hot and slightly painful to the touch. With disorders of lymph circulation, hyperemia has a cyanotic hue, with trophic disorders of the dermis with lymphovenous insufficiency – brownish. After pressing the erythema region with the fingers, the redness below them disappears for 1-2 s. Due to the stretching of the epidermis, erythema glistens, along its edges the skin is slightly raised in the form of a peripheral infiltration roller. At the same time, in most cases, especially with primary or repeated erysipelas, the phenomena of regional lymphadenitis are observed: compaction of the lymph nodes, their soreness on palpation, limitation of mobility. Many patients have concomitant lymphangitis in the form of a narrow pale pink strip on the skin, connecting erythema with a regional group of lymph nodes.
From the side of internal organs one can observe muffled heart sounds, tachycardia, arterial hypotension. In rare cases, meningeal symptoms appear.
Fever, different in height and nature of the temperature curve, and other manifestations of toxicosis usually last 5-7 days, and sometimes a little longer. With a decrease in body temperature, a period of convalescence begins. The reverse development of local inflammatory reactions occurs later than normalization of body temperature: erythema turns pale, its borders become fuzzy, and the edge infiltration roller disappears. Edema subsides, regional lymphadenitis phenomena decrease and pass. After the disappearance of hyperemia, small-scaled peeling of the skin is observed, pigmentation is possible. In some cases, regional lymphadenitis and skin infiltration persist for a long time, indicating a risk of early relapse of erysipelas. Long-term persistent edema is a sign of the formation of lymphostasis. The given clinical characteristic is characteristic of erythematic erysipelas.
Erythematous hemorrhagic erysipelas. In recent years, the condition is much more common; in some regions, by the number of cases, it comes first among all forms of the disease. The main difference between the local manifestations of this form from erythematous is the presence of hemorrhages – from petechiae to extensive drain hemorrhages against the background of erythema. The disease is accompanied by a longer fever (10-14 days or more) and a slow reverse development of local inflammatory changes. Often there are complications in the form of skin necrosis.
Erythematous-bullous erysipelas. The formation of small vesicles on the background of erythema (conflicts, noticeable in lateral illumination) or large vesicles filled with transparent serous contents is characteristic. Bubbles form several hours or even 2-3 days after the onset of erythema (due to epidermal detachment). In the dynamics of the disease, they rupture spontaneously (or they are opened with sterile scissors), the serous contents expire, the dead epidermis exfoliates. The macerated surface slowly epithelizes. Crusts form, after which no scar remains. Infectious-toxic syndrome and regional lymphadenitis do not have fundamental differences from their manifestations in erythematic erysipelas.
Bullous hemorrhagic erysipelas. The fundamental difference from erythematous-bullous erysipelas is the formation of blisters with serous-hemorrhagic contents caused by deep damage to the capillaries. When opening bubbles on a macerated surface, erosion and ulceration often form. This form is often complicated by deep necrosis, phlegmon; after recovery, scars and skin pigmentation remain.
The most frequent localization of the local inflammatory focus in erysipelas is the lower limbs, less often the face, even less often the upper limbs, chest (usually with lymphostasis in the area of postoperative scars), etc.
Erysipelas, regardless of the form of the disease, has some age-related features.
- Children get sick rarely and easily.
- In elderly people, primary and repeated erysipelas usually have a more severe course, with a prolonged febrile period (sometimes up to 4 weeks) and an exacerbation of various concomitant chronic diseases.
Regional lymphadenitis in most patients is absent. Regression of local manifestations in the elderly is slow.
The disease is prone to recurrent course. There are early (in the first 6 months) and late, frequent (3 times a year or more) and rare relapses. With frequent relapse of the disease (3-5 times a year or more) they talk about the chronic course of the disease. In these cases, quite often the symptoms of intoxication are mild, the fever is short, erythema is dull and without clear boundaries, regional lymphadenitis is absent.
Complications
The disease is often complicated by abscesses, phlegmon, deep skin necrosis, ulcers, pustulation, phlebitis and thrombophlebitis, in rare cases – pneumonia and sepsis. Due to lymphovenous insufficiency, progressing with each new relapse of the disease (especially in patients with frequently recurring erysipelas), the consequences of erysipelas in the form of lymphostasis (lymphedema) and elephantiasis (fibredema) are formed in 10-15% of cases. With a prolonged course of elephantiasis, hyperkeratosis, skin pigmentation, papillomas, ulcers, eczema, lymphorrhea develop.
Diagnosis of Erysipelas
I give birth to differentiate from many infectious, surgical, skin and internal diseases: erisipeloid, anthrax, abscess, phlegmon, panaritium, phlebitis and thrombophlebitis, obliterating endarteritis with trophic disorders, eczema, dermatitis, toxicoderma and other skin diseases, systemic lupus erythematosus, sclerosis other
When making a clinical diagnosis, erysipelas take into account the acute onset of the disease with fever and other manifestations of intoxication, more often ahead of the occurrence of typical local phenomena (in some cases occurring simultaneously with them), the characteristic localization of local inflammatory reactions (lower limbs, face, less often other areas of the skin ), the development of regional lymphadenitis, the absence of severe pain at rest.
Laboratory diagnostics
Excretion of the pathogen is usually not carried out.
Erysipelas Treatment
Perhaps outpatient treatment of erysipelas, but in some cases hospitalization is indicated. These cases include often recurring and severe forms of the disease, the presence of severe general concomitant diseases, senile or children’s age of patients.
Etiotropic therapy is carried out by prescribing penicillins (intramuscularly 4-6 million units / day), cephalosporins I and II generations (1 g 3-4 times a day), as well as some macrolides, glycopeptides, fluoroquinolones in medium therapeutic doses at a rate of 7- 10 days Erythromycin, oleandomycin, sulfanilamide and nitrofuran drugs are less effective. In case of often recurring erysipelas, sequential two-course antibiotic therapy is used: following the course of ß-lactam preparations, after a 2-3-day break, lincomycin is prescribed at 0.6 g 3 times a day intramuscularly for 7 days. Detoxification and anti-inflammatory therapy with non-steroidal anti-inflammatory drugs, antihistamines and symptomatic agents, vitamins C, B, and B6 are indicated.
Local therapy is carried out for bullous forms of erysipelas by opening the blisters and applying frequently replaced gauze napkins moistened with solutions of antiseptics (furatsilina 1: 5000, ethacridine lactate 1: 1000, dimexide, dioxidine, octanisept, etc.). The use of various ointments is limited, since they often irritate the skin, enhance exudation and slow down reparative processes. Sometimes prescribed bepanten, bepanten plus, dermazine.
To more quickly eliminate residual phenomena and prevent the effects of erysipelas, physiotherapeutic methods are used: ultraviolet radiation, UHF, ozokerite, paraffin, etc. Phyto-, laser-, and magnetotherapy methods are being developed.
In some cases, patients with erysipelas are shown anti-relapse treatment after discharge from the hospital. For this, bicillin-5 injections of 1.5 million units or retarpen of 2.4 g intramuscularly are prescribed at intervals of 3 weeks between injections. In case of often recurring erysipelas, the injection course is continued for 2 years. In patients with residual effects and a risk of relapse after discharge from the hospital, injections are performed for 3-6 months. In seasonal relapses, anti-relapse treatment is started a month before their usual onset time and is carried out for 3-4 months.
Erysipelas Prevention
It is necessary to monitor the cleanliness of the skin. Primary treatment of wounds, cracks, treatment of pustular diseases, strict adherence to asepsis during medical manipulations serve as a means of preventing erysipelas.
Activities in the outbreak
Events are not regulated. Clinical observation of convalescents of primary erysipelas is carried out in the office of infectious diseases of the clinic for 3 months; suffering from recurring erysipelas is observed for at least 2 years since the last relapse.